Catching Pelvic Floor Dysfunction, Red Handed
The Overlooked Culprit: When Pelvic Floor Dysfunction Masquerades as Endometriosis, PCOS, or UTIs, what can gynec do?
She walks in for the fifth time this year. Mid-thirties. Sharp eyes dulled by fatigue. She’s carried a folder thicker than most patient files, filled with prescriptions, ultrasound reports, and urine cultures that all whisper the same frustrating word: “normal.”
She’s had it all — antispasmodics, antibiotics, even a diagnostic laparoscopy that came up inconclusive. You’ve run the checklist. Endometriosis? Ruled out. PCOS? Not quite. UTI? Cultures clean. Yet, the pain remains. Like a ghost that shows up month after month, haunting her pelvis and confusing every specialist she meets.
It’s easy to think she’s a difficult patient. Or maybe it’s “in her head.” But what if the problem isn’t in her ovaries or uterus or bladder? What if it’s a little south of where we usually look?
This isn’t rare. In fact, it’s surprisingly common — pelvic floor dysfunction (PFD), a quiet disruptor that hides in plain sight, mimicking everything from endometriosis to urinary infections. And we, in our well-meaning algorithms of diagnosis, often miss it.
But the floor never lies. You just have to know where to look.
Pelvic Floor Dysfunction
PFD is like the chameleon of pelvic health, blending seamlessly with other conditions. It occurs when the pelvic floor muscles fail to function properly, leading to a spectrum of symptoms that can easily be mistaken for more commonly diagnosed disorders. Studies have shown that the prevalence of PFD among women varies widely, with some Indian studies reporting rates as high as 40% in rural areas.
The Great Impersonator: PFD's Many Faces
Mimicking Endometriosis
Endometriosis affects approximately 10% of women of reproductive age worldwide, which translates to about 42 million women in India. Its symptoms—dysmenorrhea, chronic pelvic pain, and dyspareunia—are strikingly similar to those of PFD. Without a thorough evaluation, it's easy to attribute these symptoms solely to endometriosis, potentially overlooking an underlying PFD.
Imitating PCOS
PCOS is characterized by hormonal imbalances, irregular menstrual cycles, and ovarian cysts. While PFD doesn't replicate these hormonal issues, the associated pelvic discomfort and menstrual irregularities can lead to diagnostic confusion. Distinguishing whether pelvic pain stems from ovarian pathology or musculoskeletal issues related to PFD is crucial.
Disguised as UTIs
Frequent urination, urgency, and pelvic discomfort are hallmark symptoms of UTIs. However, these can also arise from PFD, particularly when pelvic floor muscles are hypertonic. Recurrent UTIs with negative cultures should prompt consideration of PFD as an underlying cause.
Take, for example,
a 35-year-old woman who has been treated multiple times for suspected UTIs and evaluated for endometriosis, all with inconclusive results. A comprehensive pelvic exam reveals hypertonic pelvic floor muscles. Referral to a pelvic floor physical therapist leads to significant symptom relief after targeted therapy. This scenario underscores the importance of considering PFD in differential diagnoses.
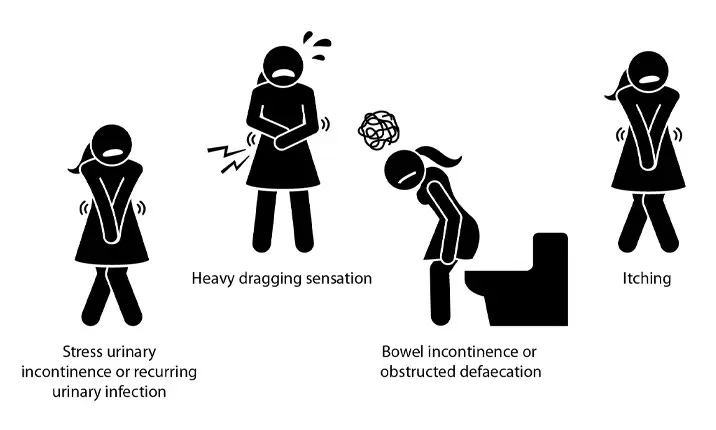
Spotting the Red Flags
To enhance diagnostic accuracy, be vigilant for the following indicators:
Chronic pelvic pain unresponsive to conventional treatments.
Dyspareunia without identifiable gynaecological pathology.
Voiding dysfunctions, such as incomplete bladder or bowel emptying.
Recurrent UTIs with negative urine cultures.
A sensation of pelvic heaviness or bulging.
Integrating Screening into Practice
Incorporating specific questions into patient evaluations can aid in identifying PFD:
Do you experience a sensation of heaviness or bulging in the pelvic area?
Do you have difficulty initiating urination or feel that your bladder isn't completely emptying?
Do you experience pain during intercourse that's not explained by other conditions?
Affirmative answers should prompt further assessment for PFD.
Building Collaborative Care
Establishing a referral network with pelvic floor physical therapists can significantly enhance patient outcomes. Collaborative care has been shown to improve women's health outcomes associated with PFD. By integrating these specialists into your practice, you offer patients comprehensive care that addresses both gynaecological and musculoskeletal components of their symptoms.
ABC of Building the Practice of Winners
Develop a referral protocol: Create a streamlined process for referring patients to trusted pelvic floor therapists.
Educate your team: Ensure that all staff members understand the signs of PFD and the benefits of physical therapy.
Patient education: Provide informational materials to patients about PFD and the role of physical therapy in treatment.
Pelvic floor dysfunction is a master of disguise, often presenting as endometriosis, PCOS, or UTIs. By maintaining a high index of suspicion and incorporating targeted screening into your practice, you can unmask this condition and guide your patients toward effective relief.
Endometriosis Weekly Update —
The Best Surgeries Are the Ones We Don’t Need– A powerful read on the complexities of endometriosis treatment. This piece dives into why surgery isn't always the best answer, the importance of expert care, and what patients should consider before going under the knife. A must-read for anyone navigating this challenging condition! 💛
Read full article here-
We are excited to announce our Fellowship in Minimal Invasive Surgery (MIS)
under the aegis of Gujarat University! This 1-year intensive program offers hands-on surgical training, live demonstrations, and research opportunities!
Fellowship Begins: 1st May 2025
📩 Apply now by sending your CV to: mims@mayflowerhospital.com
CSEEMIG IS BACK!
Some skills are not learned—they’re lived, observed in quiet moments in the OT, traced through scans, and stitched into memory with every suture.
Observe Dr. Sanjay Patel, Dr Smeet Patel and the iconic Mayflower Endo Team perform live surgeries featuring advanced techniques like the Butterfly Peritonectomy and Rule of M.
Gain insight through case discussions, Q&A sessions, and shared experiences with peers.
Registration and Payment:
Register here: https://membership.iageonline.com/Course_Home.aspx
Pay here: https://drive.google.com/file/d/1P9vyRlvly0xNI_kO6qwWdmKt4F38Ltyj/view